Insulin Resistance and Weight Loss: Why You Can't Lose Weight and What to Do
If you have been eating carefully, exercising regularly, and still watching the scale refuse to budge, you are not alone. Many women with chronic health conditions find themselves stuck in this frustrating cycle, wondering "why can't I lose weight?" no matter how hard they try.
The answer might lie in something called insulin resistance, a metabolic condition that affects how your body processes energy. Understanding this connection could be the key to finally breaking through your weight loss plateau.
What is Insulin Resistance?
To understand insulin resistance, it helps to first understand how insulin normally works in your body. When you eat carbohydrates, your digestive system breaks them down into glucose, which enters your bloodstream. Your pancreas then releases insulin, a hormone that acts like a key, unlocking the doors to your cells so glucose can enter and be used for energy.
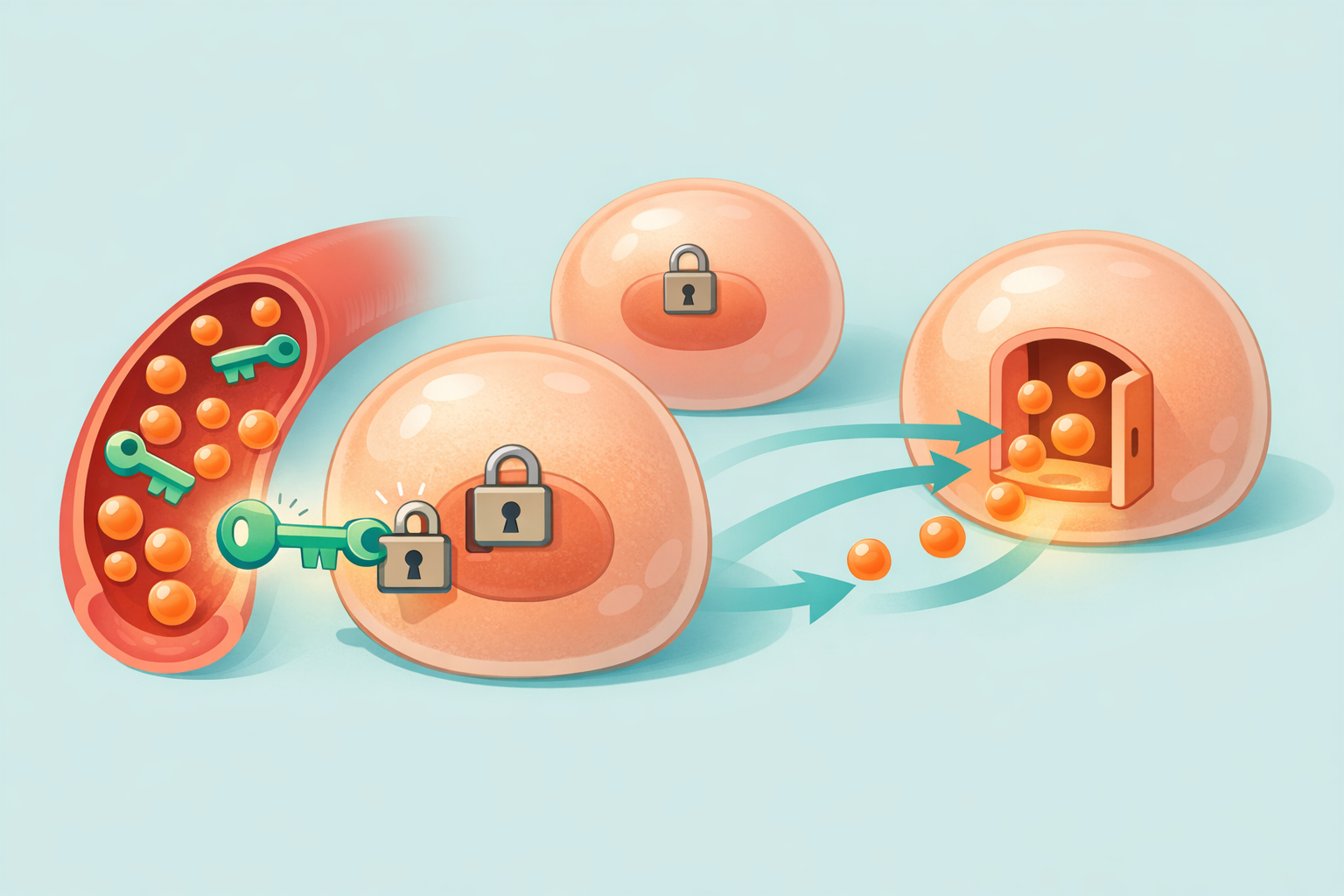
When you have insulin resistance, your cells stop responding properly to that key. The locks become stiff, and glucose cannot enter your cells as easily. Your pancreas compensates by producing even more insulin, trying to push glucose into your cells. This creates a state called hyperinsulinemia, where insulin levels remain chronically elevated.
Key takeaway: Insulin resistance means your cells do not respond efficiently to insulin, causing your body to produce excess amounts of this hormone.
Why This Makes Weight Loss Difficult
Here is where the weight loss struggle becomes clearer. Insulin is not just about blood sugar regulation. It is also a fat-storage hormone. When insulin levels are high, your body receives a signal to store fat rather than burn it. This creates a metabolic environment where losing weight becomes significantly harder, even when you are eating fewer calories.
Signs of Insulin Resistance You Should Know
Many people with insulin resistance do not realize they have it. The condition often develops gradually, and its symptoms can be mistaken for other issues or simply attributed to aging or stress. Here are common signs to watch for:
- Difficulty losing weight, especially around the midsection. This is often the most noticeable sign. You might gain weight easily but struggle tremendously to lose it, even with consistent effort.
- Fatigue after meals. Instead of feeling energized after eating, you might feel sluggish or tired, particularly after consuming carbohydrates.
- Intense sugar cravings. High insulin levels can cause blood sugar to drop rapidly, triggering cravings for sweets and refined carbohydrates.
- Dark skin patches (acanthosis nigricans). These velvety, darkened areas of skin often appear in body folds like the neck, armpits, or groin.
- Brain fog and difficulty concentrating. When your brain cells become resistant to insulin, cognitive function can suffer.
- Increased hunger and frequent hunger even after eating. Your cells are not getting the energy they need, so your body continues sending hunger signals.
Important: These symptoms can also indicate other health conditions. Only a healthcare provider can properly diagnose insulin resistance.
The Connection Between Insulin Resistance and Weight
Understanding the relationship between insulin resistance and weight requires looking at how your body handles energy. When insulin levels are consistently elevated, several things happen that make weight loss particularly challenging.
First, high insulin levels promote fat storage, especially visceral fat, the type that accumulates around your midsection and organs. This fat is metabolically active and can worsen insulin resistance, creating a frustrating cycle.
Second, elevated insulin can increase hunger and cravings, making it harder to stick with healthy eating habits. Your body might be signaling that it needs more energy, even when you have recently eaten.
Third, insulin resistance can affect how your body burns calories. Traditional "calories in, calories out" approaches may not work as effectively because insulin resistance alters your metabolic efficiency. Your body might be storing a larger percentage of the calories you consume rather than using them for energy.
This does not mean calories do not matter. Rather, it suggests that the hormonal environment in your body influences how those calories are processed and stored.
Who is at Risk for Insulin Resistance?
Several factors can increase your likelihood of developing insulin resistance. Understanding your risk factors can help you take preventive action.
- Polycystic ovary syndrome (PCOS). Women with PCOS have a significantly higher risk of insulin resistance, affecting up to 70% of those with the condition.
- Family history of type 2 diabetes. Genetics play a substantial role in how your body processes insulin.
- Sedentary lifestyle. Physical inactivity reduces your cells' sensitivity to insulin.
- Chronic stress. Ongoing stress elevates cortisol, which can interfere with insulin function.
- Poor sleep quality. Even short-term sleep deprivation can reduce insulin sensitivity.
- Certain medications. Some medications, including certain antidepressants and steroids, can affect insulin sensitivity.
- Age. Risk increases after age 45, though insulin resistance is increasingly seen in younger adults.
- Excess weight, particularly around the abdomen. Visceral fat releases inflammatory compounds that can worsen insulin resistance.
How to Reverse Insulin Resistance Through Diet
While insulin resistance can feel discouraging, the good news is that lifestyle changes, particularly dietary modifications, can significantly improve insulin sensitivity. An insulin resistance diet focuses on stabilizing blood sugar and reducing the demand for insulin.
Foods That Improve Insulin Sensitivity

Building your meals around these foods can help your cells become more responsive to insulin:
Fiber-rich vegetables
- Leafy greens like spinach, kale, and Swiss chard
- Cruciferous vegetables such as broccoli, cauliflower, and Brussels sprouts
- Bell peppers, zucchini, and green beans
- Artichokes and asparagus
Lean proteins
- Chicken breast and turkey
- Fish, especially fatty fish like salmon and mackerel
- Eggs
- Legumes such as lentils and chickpeas
- Tofu and tempeh
Healthy fats
- Avocados
- Nuts, particularly almonds and walnuts
- Seeds like chia, flax, and pumpkin seeds
- Extra virgin olive oil
- Fatty fish
Whole grains in moderation
- Quinoa
- Brown rice
- Steel-cut oats
- Barley
Foods rich in magnesium and chromium
- Dark leafy greens
- Pumpkin seeds
- Dark chocolate (in moderation)
- Broccoli
- Grape juice (unsweetened, small amounts)
Key takeaway: Focus on foods that cause a gradual, modest rise in blood sugar rather than rapid spikes.
Foods to Limit or Avoid with Insulin Resistance
Certain foods can worsen insulin resistance by causing sharp spikes in blood sugar and increasing insulin demand:
- Refined carbohydrates. White bread, white rice, pastries, and most crackers cause rapid blood sugar increases.
- Sugary beverages. Soda, sweetened teas, fruit juices, and energy drinks deliver large amounts of sugar quickly.
- Processed snacks. Chips, cookies, candy bars, and most packaged snack foods often combine refined carbs with unhealthy fats.
- Excessive alcohol. Alcohol can affect blood sugar regulation and liver function.
- Added sugars. Watch for hidden sugars in sauces, dressings, and supposedly healthy foods like flavored yogurts.
You do not need to eliminate these foods entirely forever. However, reducing their intake can significantly improve how your body responds to insulin.
Meal Timing Strategies for Better Blood Sugar Control
When and how you eat matters as much as what you eat for managing insulin resistance.
Build balanced meals. Each meal should include protein, healthy fats, and fiber-rich carbohydrates. This combination slows digestion and prevents sharp blood sugar spikes. A balanced plate might include grilled salmon (protein), roasted vegetables (fiber), quinoa (complex carbs), and a drizzle of olive oil (healthy fat).
Avoid skipping meals. Going long periods without eating can cause blood sugar to drop, leading to intense hunger and potential overeating later. Regular meals help keep blood sugar stable.
Consider meal spacing. Some research suggests that spacing meals 4-5 hours apart allows insulin levels to return to baseline between meals, which may improve insulin sensitivity over time.
Explore time-restricted eating cautiously. Some studies show benefits from eating within a compressed window, such as 8-10 hours. However, this approach is not suitable for everyone, particularly those with certain medical conditions or a history of disordered eating. Always consult a healthcare provider before trying this approach.
Beyond Diet: Lifestyle Changes That Improve Insulin Sensitivity

While nutrition is foundational, other lifestyle factors significantly influence insulin sensitivity.
Resistance training. Building muscle through strength training increases the number of cells that can absorb glucose from your bloodstream. Muscle tissue is highly metabolically active and improves insulin sensitivity even when you are not exercising.
Walking after meals. A 10-15 minute walk after eating can help your muscles use glucose from your meal, reducing the insulin demand on your body. This simple habit can make a meaningful difference over time.
Stress management. Chronic stress keeps cortisol elevated, which can worsen insulin resistance. Gentle practices like deep breathing, meditation, yoga, or simply spending time in nature can help.
Prioritizing sleep. Poor sleep reduces insulin sensitivity and increases cravings for high-carbohydrate foods. Aim for 7-9 hours of quality sleep by maintaining a consistent bedtime, limiting screens before bed, and creating a dark, cool sleeping environment.
Key takeaway: Combining dietary changes with regular movement, stress reduction, and quality sleep creates the best environment for improving insulin sensitivity.
When to See a Healthcare Provider
If you suspect you might have insulin resistance, speaking with a healthcare provider is important. Several tests can help assess your metabolic health:
- Fasting insulin test. This measures insulin levels after an overnight fast. Elevated fasting insulin can indicate insulin resistance, often before blood sugar levels become abnormal.
- HOMA-IR. The Homeostatic Model Assessment of Insulin Resistance is a calculated value based on your fasting glucose and insulin levels.
- Hemoglobin A1C. This test shows your average blood sugar over the past 2-3 months and can identify prediabetes or diabetes.
- Oral glucose tolerance test. This measures how your body handles a set amount of glucose over time.
Do not wait until you develop prediabetes or type 2 diabetes to investigate. Early detection allows for earlier intervention.
Ask your doctor about these tests if you have risk factors for insulin resistance or are experiencing symptoms. Keep in mind that standard blood work might not always include fasting insulin, so you may need to specifically request it.
How a Dietitian Can Help with Insulin Resistance
Managing insulin resistance through diet can feel overwhelming, especially when you are already dealing with other health conditions. This is where working with a registered dietitian can make a significant difference.
A dietitian can help you create a personalized eating plan that considers your specific health conditions, food preferences, lifestyle, and goals. They can also help you navigate conflicting nutrition information and provide accountability and support.
Generic calorie-tracking apps offer AI-generated advice, but they cannot account for the full complexity of your health history or provide the nuanced guidance that insulin resistance often requires. Working with a qualified professional ensures you receive evidence-based recommendations tailored to your unique situation.
Taking the Next Step
Insulin resistance is a manageable condition. With the right combination of nutrition, movement, stress management, and sleep, many people see significant improvements in their insulin sensitivity and find that weight loss becomes more achievable.
Progress may be gradual, and that is okay. Focus on consistency rather than perfection. Small, sustainable changes often lead to more lasting results than dramatic overhauls.
If you are ready for personalized support, Kukta AI connects you with registered dietitians who specialize in metabolic health and can create an individualized plan for your needs. Kukta AI empowers real, local, registered dietitians with artificial intelligence so they can help clients with the most modern technologies available. Unlike generic calorie-tracking apps that only offer AI-generated advice, Kukta AI is the first platform that connects users with a large community of international, registered, vetted dietitians supported by AI tools.
Always consult with a healthcare professional or registered dietitian before making significant changes to your diet or exercise routine, especially if you have existing health conditions or take medications.
Your journey to better metabolic health is worth the effort, and you do not have to navigate it alone.